TMJ stands for Temporomandibular Joint Disorder which affects the jaw joint together with nearby muscles that frequently result in problems with pain alongside stiffness or movement issues. The condition produces serious effects on basic necessary activities such as chewing and speaking. Proper management and prevention of TMJ require identifying its underlying factors. The following article analyzes typical TMJ triggers by showing their development sources while presenting methods for handling and preventing these precursors.
Anatomy of the Temporomandibular Joint (TMJ)

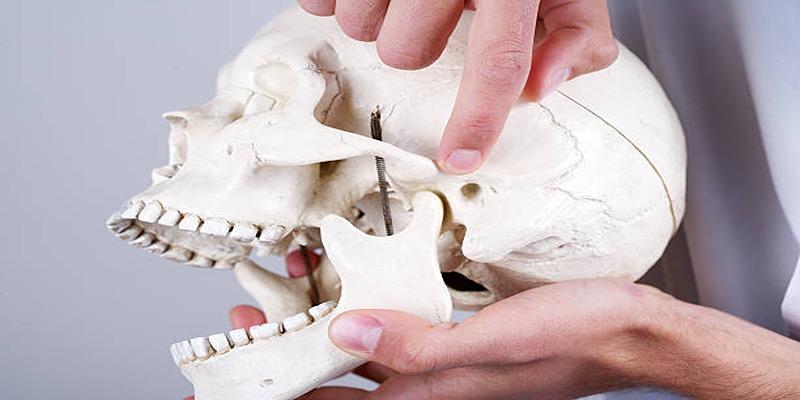
Knowledge about the structures of temporomandibular joints is necessary for comprehending their source factors. Two points on each side of the head unite the jawbone through a hinge joint with the skull. The connection between jawbone and skull enables these functions: mouthing movements and chewing and all aspects of speech.
The TMJ also has a disc made of cartilage that acts as a cushion between the bones, allowing for smooth movement and absorbing shock. Surrounding muscles and ligaments help support and stabilize this joint during movement.
Common Causes
Temporomandibular joint (TMJ) disorders can arise from various causes, leading to discomfort and difficulty in jaw movement.
1. Trauma or Injury
Direct trauma to the jaw or surrounding areas can significantly impact the TMJ. This includes incidents such as falls, car accidents, or sports injuries. Even subtle, repetitive stress from habits like teeth clenching can contribute to damage over time. Injuries may lead to inflammation, misalignment, or structural damage, restricting normal joint movement and resulting in pain or clicking sounds during activities like chewing or speaking.
2. Arthritis
Arthritis, particularly osteoarthritis or rheumatoid arthritis, can affect the TMJ. Osteoarthritis is caused by wear and tear over time, leading to the breakdown of cartilage within the joint. Rheumatoid arthritis, on the other hand, results from the immune system attacking joint tissues, causing inflammation. Both conditions can result in limited jaw movement, pain, and stiffness, impacting daily functions such as eating and talking. Early diagnosis and management are crucial in preventing further joint degradation.
3. Teeth Grinding or Clenching
Bruxism, or teeth grinding and clenching, places excessive pressure on the TMJ. This habit often occurs during sleep and may go unnoticed initially. Over time, this constant strain fatigues the jaw muscles, leading to inflammation or joint imbalance. It may also result in tooth damage, exacerbating pressure on the joint. Treatment options, such as stress management or wearing a mouthguard, are often effective in mitigating the impact of bruxism on the TMJ.
4. Poor Posture
Sitting or standing with poor posture can impact the alignment and balance of the TMJ, leading to muscle tension and strain. Similarly, habits like cradling a phone between the ear and shoulder can place excessive stress on one side of the jaw, contributing to joint dysfunction. Practicing good posture techniques, such as keeping the head aligned with the spine and avoiding prolonged positions that strain the neck or shoulders, can help alleviate pressure on the TMJ.
Symptoms Associated with TMD
TMD, or temporomandibular joint disorder, can produce a variety of symptoms that affect the jaw, face, and surrounding areas.
1. Jaw Pain and Tenderness
One of the hallmark symptoms of TMD is persistent pain or tenderness in the jaw. This discomfort can be localized around the TMJ or radiate through the face, neck, or shoulders. It is often aggravated by movements such as chewing or speaking, and the intensity may vary throughout the day. Prompt evaluation of jaw pain can aid in identifying underlying TMD and initiating effective treatment.
2. Limited Range of Motion
Individuals with TMD often experience difficulty opening their mouths fully or smoothly. This restriction in movement may impede daily activities, such as eating or speaking, and is sometimes accompanied by a sensation of the jaw "locking" in position. The limited range of motion can worsen over time if not addressed, making it essential to consult with healthcare providers for interventions that promote proper joint function and mobility.
3. Clicking or Popping Sounds
Another common sign of TMD is audible clicking, popping, or grating sounds emanating from the jaw joint during movement. These sounds, while not always painful, may indicate misalignment or inflammation within the joint. Over time, these noises can become more pronounced, particularly during activities that involve significant jaw movement, such as eating or speaking. Monitoring these symptoms can help determine the severity and progression of TMD.
4. Headaches or Ear Pain
TMD can also cause referred pain, leading to headaches, earaches, or pressure in the ears. This is due to the proximity of the TMJ to other structures in the head and face and may be exacerbated by tension within the jaw muscles. It is vital to differentiate TMD-related pain from other causes through proper evaluation and diagnosis.
Treatment Options

Treatment options for TMD vary depending on symptom severity and underlying causes. Below are some common approaches to managing this condition.
1. Lifestyle Modifications
Simple lifestyle changes can significantly alleviate TMD symptoms. Avoiding hard or chewy foods, reducing stress through relaxation techniques, and refraining from behaviors like clenching or teeth grinding can minimize jaw strain. Incorporating regular gentle jaw exercises may also improve mobility and reduce stiffness over time. These adjustments, when combined with mindfulness of jaw posture, can play an essential role in managing the condition effectively and preventing further discomfort.
2. Medication
Over-the-counter pain relievers or anti-inflammatory medications, like ibuprofen, can help manage mild symptoms. For more severe cases, healthcare providers may prescribe muscle relaxants to ease tension or corticosteroid injections to reduce inflammation in the temporomandibular joint. Topical analgesics, such as numbing creams, may offer localized relief. Medications are typically part of a broader treatment plan, intended to facilitate more immediate relief while other therapies address the condition's root causes.
3. Physical Therapy
Physical therapy is an effective treatment for improving jaw function and reducing pain. A physical therapist may use specialized techniques like stretching, strengthening exercises, and massage to relieve tension in the jaw and surrounding muscles. Therapy may also include ultrasound or heat treatments to enhance circulation and promote healing. Consistent physical therapy sessions can lead to improved alignment, better movement, and long-term symptom management for individuals living with TMD.
Conclusion
TMD treatment often requires a multifaceted approach involving medical, therapeutic, and lifestyle interventions. With timely diagnosis and a personalized treatment plan, most individuals can achieve significant symptom relief and improved quality of life. Whether through medication, physical therapy, or other techniques, addressing TMD effectively ensures better jaw function and overall well-being. It’s essential to work closely with healthcare providers to identify the best options for managing the condition and promoting long-term recovery.